Lagans Wellness Clinic has Low Level Laser Therapy, which can help speed up Mum's recovery.
When is low level laser therapy useful?

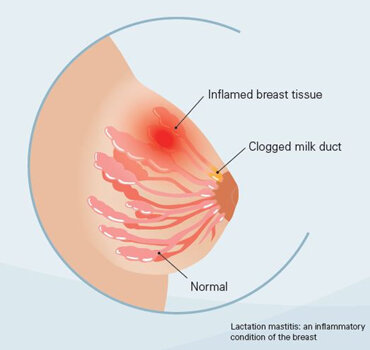
Mastitis is an inflammation of breast tissue that sometimes involves an infection. The inflammation results in breast pain and tenderness, swelling, warmth and redness. Mastitis most commonly affects women who are breast-feeding (lactation mastitis), but can also occur in women who aren’t breast-feeding and in men.
Low Level Laser Therapy or Photobiomodulation Therapy significantly reduces or eliminates inflammation. The oedema (engorgement or swelling) associated with this condition is also reduced or eliminated, generating healthy breast tissue. This reduction in pain and swelling is likely to encourage continuation of breastfeeding.
One of the major effects of light when absorbed by our bodies, is on the mitochondria, the power source inside our cells. When cells are stressed through injury or damage, the mitochondria produce nitric oxide (a toxic chemical), which in turn reduces oxygen production, significantly lowering cell energy and leading to a state of oxidative stress. Oxidative stress then creates a state of inflammation and cell death. LLLT or PMB Therapy dissociates the nitric oxide allowing oxygen back into the cell, so the energy level of the cell is restored and oxidative stress is reduced. Once normal mitochondrial function is re-established through LLLT, cell function improves, pain reduces and the patient begins to feel better.
Breastfeed Rev. 2016 Jul;24(2):27-31.
Buck ML, Eckereder G, Amir LH.
Breast and nipple pain, nipple damage and mastitis are common reasons given by women for their early cessation of breastfeeding. There are a limited number of effective therapies available to support healing of damaged nipples during lactation. Low level laser therapy is a painless treatment, which appears to accelerate wound healing and ease pain. We present two case studies, which demonstrate the use of low level laser therapy in clinical practice.
PMID:29211392[Indexed for MEDLINE]
and
Pain Manag Nurs. 2016 Aug;17(4):281-9. doi: 10.1016/j.pmn.2016.05.003. Epub 2016 Jun 27.
Coca KP1, Marcacine KO2, Gamba MA2, Corrêa L3, Aranha AC3, Abrão AC2.
1Escola Paulista de Enfermagem, Universidade Federal de São Paulo, São Paulo, Brazil. Electronic address: kcocaepm@hotmail.com.2Escola Paulista de Enfermagem, Universidade Federal de São Paulo, São Paulo, Brazil.3Faculdade de Odontologia, Universidade de São Paulo, São Paulo, Brazil.
Pain accruing from nipple lesions caused by inadequate latching by the baby is a common complaint among breastfeeding women and an important obstacle to successful breastfeeding. Nipple pain occurs during the first days after delivery and is considered one of the main causes for early weaning. To investigate the efficacy of low-level laser therapy as a treatment for nipple pain due to breastfeeding. A triple-blind, randomized, clinical study. A university-affiliated hospital in São Paulo, Brazil. Fifty-nine women with nipple lesions at the time of their admission. Thirty women (intervention group) received three sessions of laser therapy (InGaAIP laser, 660 nanometer, 40 milliwatts of power, 5 Joules per square centimeter of energy density for 5 seconds each, total energy = 0.6 Joules) in the region of the nipples at three different points in time (0 hour, 24 hours, and 48 hours after diagnosis of nipple lesion). Twenty-nine women with similar clinical conditions were randomly assigned to the control group. Self-reported pain was recorded before and after laser therapy using a visual analogue scale. The intervention group experienced a decrease of 2.0 centimeters in intensity of pain (p = .016) 24 hours after the first intervention and also presented lower levels of pain compared with the control group. Low-level laser therapy was considered effective for treating nipple lesions in breastfeeding women with pain, providing relief and prolonging exclusive breastfeeding. More clinical trials with different laser dosimetry and parameters are necessary to optimize laser therapy protocols for breastfeeding women.
Copyright © 2016 American Society for Pain Management Nursing. Published by Elsevier Inc. All rights reserved.
PMID:27363734DOI:10.1016/j.pmn.2016.05.003[Indexed for MEDLINE]